REVIEW PAPER
Postpartum depression in men – a common but rarely understood problem
1
Students’ Scientific Circle at the Department of Applied Psychology, Medical University, Lublin, Poland
2
Department of Applied Psychology, Medical University, Lublin, Poland
Corresponding author
Magdalena Leśniewska
Studenckie Koło Naukowe przy Zakładzie Psychologii Stosowanej, Uniwersytet Medyczny w Lublinie, ul.Chodźki 7, 20-093, Lublin, Polska
Studenckie Koło Naukowe przy Zakładzie Psychologii Stosowanej, Uniwersytet Medyczny w Lublinie, ul.Chodźki 7, 20-093, Lublin, Polska
Med Og Nauk Zdr. 2021;27(3):248-251
KEYWORDS
TOPICS
ABSTRACT
Introduction:
Postpartum depression (PPPD) is defined as the occurrence of a depressive episode in the postpartum period, with a peak incidence between 3–6 months. It is estimated that 1 in 10 fathers are currently affected, yet most research focuses only on postpartum depression in mothers.
Objective:
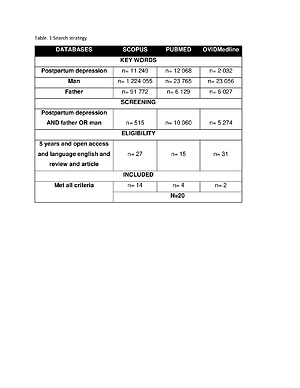
The aim of the study was to analyze scientific reports on paternal postpartum depression in men. The available literature on ‘postpartum depression among men’ was reviewed based on the Scopus, PubMed and OVIDMedline databases.
Brief description of the state of knowledge:
The questionnaire useiIn the diagnosis of PPPD is the Edinburgh Postnatal Depression Scale (EPDS), a screening test for postnatal depression occurring in mothers, but it has also found application in fathers
Results:
Fathers perceived a lack of perinatal health care education in relation to their needs and a shortage of specialist support. The father’s disturbed mental state prevents him from taking full responsibility for the family and places a mental strain on the mother. At the same time, a poor partner relationship is a risk factor for PPPD. Paternal PPD is a danger to newborn children who are at a critical stage of their development
Conclusions:
Fathers should be screened for early detection of PPPD and intervention in a disorder that lacks appropriate diagnostic tools. Public awareness of PPPD is important because fathers are particularly vulnerable, and can be lacking in meeting traditional expectations and modern fatherhood tasks.
Postpartum depression (PPPD) is defined as the occurrence of a depressive episode in the postpartum period, with a peak incidence between 3–6 months. It is estimated that 1 in 10 fathers are currently affected, yet most research focuses only on postpartum depression in mothers.
Objective:
The aim of the study was to analyze scientific reports on paternal postpartum depression in men. The available literature on ‘postpartum depression among men’ was reviewed based on the Scopus, PubMed and OVIDMedline databases.
Brief description of the state of knowledge:
The questionnaire useiIn the diagnosis of PPPD is the Edinburgh Postnatal Depression Scale (EPDS), a screening test for postnatal depression occurring in mothers, but it has also found application in fathers
Results:
Fathers perceived a lack of perinatal health care education in relation to their needs and a shortage of specialist support. The father’s disturbed mental state prevents him from taking full responsibility for the family and places a mental strain on the mother. At the same time, a poor partner relationship is a risk factor for PPPD. Paternal PPD is a danger to newborn children who are at a critical stage of their development
Conclusions:
Fathers should be screened for early detection of PPPD and intervention in a disorder that lacks appropriate diagnostic tools. Public awareness of PPPD is important because fathers are particularly vulnerable, and can be lacking in meeting traditional expectations and modern fatherhood tasks.
REFERENCES (24)
1.
Scarff JR. Postpartum Depression in Men. Innov Clin Neurosci. 2019; 16(5–6): 11–14. PMID: 31440396; PMCID: PMC6659987.
2.
Soliday E, McCluskey-Fawcett K, O'Brien M. Postpartum affect and depressive symptoms in mothers and fathers. Am J Orthopsychiatry. 1999; 69(1): 30–8. https://doi.org/10.1037/h00803....
3.
Koch S, De Pascalis L, Vivian F, Meurer Renner A, Murray L, Arteche A. Effects of male postpartum depression on father-infant interaction: The mediating role of face processing. Infant Ment Health J. 2019; 40(2): 263–276. https://doi.org/10.1002/imhj.2....
4.
Johansson M, Benderix Y, Svensson I. Mothers' and fathers' lived experiences of postpartum depression and parental stress after childbirth: a qualitative study. Int J Qual Stud Health Well-being. 2020; 15(1): 1722564. https://doi.org/10.1080/174826....
5.
Leach LS, Poyser C, Cooklin AR, Giallo R. Prevalence and course of anxiety disorders (and symptom levels) in men across the perinatal period: A systematic review. J Affect Disord. 2016; 190: 675–686. https://doi.org/10.1016/j.jad.....
6.
Cameron EE, Sedov ID, Tomfohr-Madsen LM. Prevalence of paternal depression in pregnancy and the postpartum: An updated meta-analysis. J Affect Disord. 2016; 206: 189–203. https://doi.org/10.1016/j.jad.....
7.
Albicker J, Hölzel LP, Bengel J, Domschke K, Kriston L, Schiele MA, Frank F. Prevalence, symptomatology, risk factors and healthcare services utilization regarding paternal depression in Germany: study protocol of a controlled cross-sectional epidemiological study. BMC Psychiatry. 2019; 19(1): 289. https://doi.org/10.1186/s12888....
8.
Cameron EE, Hunter D, Sedov ID, Tomfohr-Madsen LM. What do dads want? Treatment preferences for paternal postpartum depression. J Affect Disord. 2017; 215: 62–70. https://doi.org/10.1016/j.jad.....
9.
Francisca Pérez C, Anthea Catalán, Alyson Morales, Antonia Quinlan, Diego Riquelme, Javiera Navarro, Camila Valdés.Assessment of Postpartum Depression in a Group of Chilean Parents. Journal of Men's Health. 2018. 14(2); 56–64. https://doi.org/10.22374/1875-....
10.
Shaheen NA, AlAtiq Y, Thomas A, Alanazi HA, AlZahrani ZE, Younis SAR, Hussein MA. Paternal Postnatal Depression Among Fathers of Newborn in Saudi Arabia. Am J Mens Health. 2019; 13(1): 1557988319831219. ht t ps://doi.org /10.1177/1557988319831219.
11.
Loscalzo Y, Giannini M, Contena B, Gori A, Benvenuti P. The Edinburgh Postnatal Depression Scale for Fathers: A contribution to the validation for an Italian sample. Gen Hosp Psychiatry. 2015; 37(3): 251–6. https://doi.org/10.1016/j.genh....
12.
Mayers A, Hambidge S, Bryant O, et al. Supporting women who develop poor postnatal mental health: what support do fathers receive to support their partner and their own mental health?. BMC Pregnancy Childbirth 20; 359(2020). https://doi.org/10.1186/s12884....
13.
Hughes C, Foley S, Devine RT, Ribner A, Kyriakou L, Boddington L, Holmes EA; NewFAMS team Creators/Copyright Holders; NewFAMS team Contributors. Worrying in the wings? Negative emotional birth memories in mothers and fathers show similar associations with perinatal mood disturbance and delivery mode. Arch Womens Ment Health. 2020; 23(3): 371–377. https://doi.org/10.1007/s00737....
14.
Psouni E, Agebjörn J, Linder H. Symptoms of depression in Swedish fathers in the postnatal period and development of a screening tool. Scand J Psychol. 2017; 58(6): 485–496. https://doi.org/10.1111/sjop.1....
15.
Schipper-Kochems S, Fehm T, Bizjak G, Fleitmann AK, Balan P, Hagenbeck C, Schäfer R, Franz M. Postpartum Depressive Disorder – Psychosomatic Aspects. Geburtshilfe Frauenheilkd. 2019; 79(4): 375–381. https://doi.org/10.1055/a-0759....
16.
Letourneau N, Leung B, Ntanda H, Dewey D, Deane AJ, Giesbrecht GF; APrON Team. Maternal and paternal perinatal depressive symptoms associate with 2- and 3-year-old children's behaviour: findings from the APrON longitudinal study. BMC Pediatr. 2019; 19(1): 435. https://doi.org/10.1186/s12887....
17.
Gutierrez-Galve L, Stein A, Hanington L, Heron J, Ramchandani P. Paternal depression in the postnatal period and child development: mediators and moderators. Pediatrics. 2015; 135(2): e339–47. https://doi.org/10.1542/peds.2....
18.
Paulson JF, Bazemore SD. Prenatal and postpartum depression in fathers and its association with maternal depression: a meta-analysis. JAMA. 2010; 303(19): 1961–9. https://doi.org/10.1001/jama.2....
19.
Cao H, Yuan X, Fine M, Zhou N, Fang X. Neuroticism and Marital Satisfaction During the Early Years of Chinese Marriage: The Mediating Roles of Marital Attribution and Aggression. Fam Process. 2019; 58(2): 478– 495. ht t ps://doi.org /10.1111/fa mp.12356.
20.
Kiviruusu O, Pietikäinen JT, Kylliäinen A, Pölkki P, Saarenpää-Heikkilä O, Marttunen M, Paunio T, Paavonen EJ. Trajectories of mothers' and fathers' depressive symptoms from pregnancy to 24 months postpartum. J Affect Disord. 2020; 260: 629–637. https://doi.org/10.1016/j.jad.....
21.
Bamishigbin ON Jr, Wilson DK, Abshire DA, Mejia-Lancheros C, Dunkel Schetter C. Father Involvement in Infant Parenting in an Ethnically Diverse Community Sample: Predicting Paternal Depressive Symptoms. Front Psychiatry. 2020; 11: 578688. https://doi.org/10.3389/fpsyt.....
22.
Edward KL, Giandinoto JA, Stephenson J, Mills C, Mcfarland J, Castle DJ. Self- screening using the Edinburgh postnatal depression scale for mothers and fathers to initiate early help seeking behaviours. Arch Psychiatr Nurs. 2019; 33(4): 421–427. https://doi.org/10.1002/da.204....
23.
Wells MB, Massoudi P, Bergström M. Swedish child health nurses treat fathers more equally in 2014 than 2004, but mothers remain their primary focus. Acta Paediatr. 2017; 106(8): 1302–1308. https://doi.org /10.1111/apa.13898.
24.
Missler M, Beijers R, Denissen J, van Straten A. Effectiveness of a psycho-educational intervention to prevent postpartum parental distress and enhance infant well-being: study protocol of a randomized controlled trial. Trials. 2018; 19(1): 4. https://doi.org/10.1186/s13063....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.