RESEARCH PAPER
The epidemiology of the testicular cancer in Poland in 2015–2021
1
Faculty of Health Sciences and Psychology, University of Rzeszów, Poland
2
Faculty of Health Sciences and Psychology, University of Rzeszów, Polska
Corresponding author
Piotr Stanisław Choręza
Department of Medical Statistics, Medical University, Ostrogórska 30 Street, 41-200 Sosnowiec, Poland
Department of Medical Statistics, Medical University, Ostrogórska 30 Street, 41-200 Sosnowiec, Poland
Med Og Nauk Zdr. 2026;32(1):36-41
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
Testicular cancer is a rare cancer constituting approximately 1% of all cancers diagnosed in men worldwide. Simultaneously the burden of the testicular cancer increased in last decades, becoming the most frequent cancer diagnosed among adolescents and young males aged 14 – 44 years of live. Our study was aimed to present the epidemiology and assess the impact of COVID-19 pandemic on the testicular cancer morbidity in Poland.
Material and methods:
The secondary epidemiological data obtained from the National Health Fund of Poland regarding males aged over 20 years of life diagnosed with the testicular cancer who have obtained healthcare services in at least one of the over 250 specialized healthcare services provided to cancer patients were analysed. The incidence rate per 100,000 males standardized to the European Standard Population 2013 (SIR) was calculated divided into subregions, according to patients’ domicile.
Results:
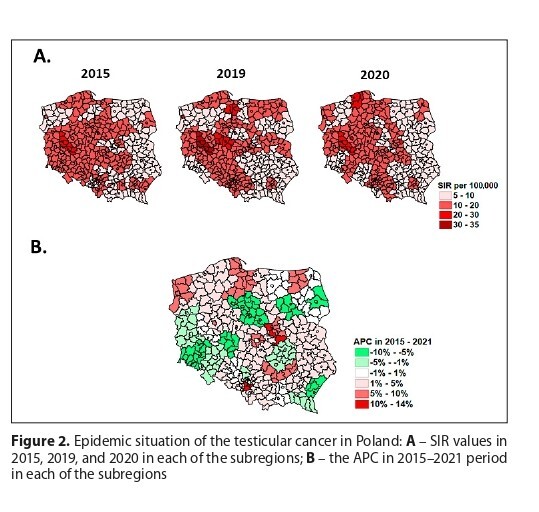
In 2015 – 2021, the average national testicular cancer incidence rate remained stable, but in 2021, an almost 10% increase in incidence compared to 2020 was noted. Furthermore, an epidemiological analysis conducted at the subregional level pointed out an increase in testicular cancer incidence in 52 of the 73 subregions, with spatial differantiation. The largest increases in incidence were observed in the Żyrardów, Tychy, and Tricity subregions, with differences between the subregions with the lowest and highest incidence.
Conclusions:
The incidence of testicular cancer in Poland in 2015 – 2021 increased despite the pandemic restrictions and limited availability of in-patient healthcare services. The spatial differentiation of incidence’s annual percent change was also demonstrated identifying areas where health promotion and health education activities should be intensified.
Testicular cancer is a rare cancer constituting approximately 1% of all cancers diagnosed in men worldwide. Simultaneously the burden of the testicular cancer increased in last decades, becoming the most frequent cancer diagnosed among adolescents and young males aged 14 – 44 years of live. Our study was aimed to present the epidemiology and assess the impact of COVID-19 pandemic on the testicular cancer morbidity in Poland.
Material and methods:
The secondary epidemiological data obtained from the National Health Fund of Poland regarding males aged over 20 years of life diagnosed with the testicular cancer who have obtained healthcare services in at least one of the over 250 specialized healthcare services provided to cancer patients were analysed. The incidence rate per 100,000 males standardized to the European Standard Population 2013 (SIR) was calculated divided into subregions, according to patients’ domicile.
Results:
In 2015 – 2021, the average national testicular cancer incidence rate remained stable, but in 2021, an almost 10% increase in incidence compared to 2020 was noted. Furthermore, an epidemiological analysis conducted at the subregional level pointed out an increase in testicular cancer incidence in 52 of the 73 subregions, with spatial differantiation. The largest increases in incidence were observed in the Żyrardów, Tychy, and Tricity subregions, with differences between the subregions with the lowest and highest incidence.
Conclusions:
The incidence of testicular cancer in Poland in 2015 – 2021 increased despite the pandemic restrictions and limited availability of in-patient healthcare services. The spatial differentiation of incidence’s annual percent change was also demonstrated identifying areas where health promotion and health education activities should be intensified.
REFERENCES (28)
1.
Filippou P, Ferguson JE 3rd, Nielsen ME. Epidemiology of Prostate and Testicular Cancer. Semin Intervent Radiol. 2016;33(3):182–185. doi:10.1055/s-0036-1586146.
2.
Khan MR, Kearney Sheehan P, Bazin A, et al. Impact of Testicular Cancer on the Socio-Economic Health, Sexual Health, and Fertility of Survivors-A Questionnaire Based Survey. Cancers (Basel). 2025;17(11):1826. doi:10.3390/cancers17111826.
3.
Raggi D, Chakrabarti D, Cazzaniga W, et al. Management of Testicular Cancer. JCO Oncol Pract 2025: OP2500211. doi:10.1200/OP-25-00211.
4.
Znaor A, Skakkebaek NE, Rajpert-De Meyts E, et al. Testicular cancer incidence predictions in Europe 2010–2035: A rising burden despite population ageing. Int J Cancer. 2020;147(3):820–828. doi:10.1002/ijc.32810.
5.
Huang J, Chan SC, Tin MS, et al. Worldwide Distribution, Risk Factors, and Temporal Trends of Testicular Cancer Incidence and Mortality: A Global Analysis. Eur Urol Oncol. 2022;5(5):566–576. doi:10.1016/j.euo.2022.06.009.
6.
Huyghe E, Matsuda T, Thonneau P. Increasing incidence of testicular cancer worldwide: a review. J Urol. 2003;170(1):5–11. doi:10.1097/01.ju.0000053866.68623.da.
7.
Moger TA, Aalen OO, Heimdal K, Gjessing HK. Analysis of testicular cancer data using a frailty model with familial dependence. Stat Med. 2004;23(4):617–632. doi:10.1002/sim.1614.
8.
Bray F, Richiardi L, Ekbom A, et al. Trends in testicular cancer incidence and mortality in 22 European countries: continuing increases in incidence and declines in mortality. Int J Cancer. 2006;118(12):3099–3111. doi:10.1002/ijc.21747.
9.
Tateo V, Thompson ZJ, Gilbert SM, et al. Epidemiology and Risk Factors for Testicular Cancer: A Systematic Review. Eur Urol. 2025;87(4):427–441. doi:10.1016/j.eururo.2024.10.023.
10.
Zhu N, Zhang D, Wang W, et al. China Novel Coronavirus Investigating and Research Team. A Novel Coronavirus from Patients with Pneumonia in China, 2019. N Engl J Med. 2020;382(8):727–733. doi:10.1056/NEJMoa2001017.
11.
Choręza PS, Kruk W, Chudek J, Owczarek AJ. The COVID-19 pandemic and epidemiology of the most common cancers in the Subcarpathian and Silesian Provinces of Poland. Ann Agric Environ Med. 2023;30(1):90–104. doi:10.26444/aaem/155304.
12.
Choręza P, Owczarek AJ, Kruk W, Chudek J. The epidemiology of the most frequent cancers in Poland in 2015–2021 and the impact of the COVID-19 pandemic on cancer incidence. Arch Public Health. 2024;82(1):49. doi:10.1186/s13690-024-01277-6.
13.
Choręza P, Owczarek AJ, Chudek J. Have Polish women started getting tested? Epidemiology of gynaecological cancers in Poland in 2015–2021. J Public Health (Berl.). 2025. doi.org/10.1007/s10389-025-02524-y.
14.
Cayuela L, Cabrera Fernández S, Roldán Testillano R, et al. Mapping regional disparities in testicular cancer mortality across Spain (2004–2023). Actas Urol Esp (Engl Ed). 2025;501800. doi:10.1016/j.acuroe.2025.501800.
15.
Statistics Poland. Local Data Bank / Główny Urząd Statystyczny. Bank Danych Lokalnych. Statistics Poland, Warsaw. URL:https://bdl.stat.gov.pl/BDL/ start (accessed: 2025.05.29).
16.
Cheng L, Albers P, Berney DM, et al. Testicular cancer. Nat Rev Dis Primers. 2018;4(1):29. doi:10.1038/s41572-018-0029-0.
17.
Ondrusova M, Ondrus D. Epidemiology and treatment delay in testicular cancer patients: a retrospective study. Int Urol Nephrol. 2008;40(1):143–148. doi:10.1007/s11255-007-9245-3.
18.
Ghazarian AA, Kelly SP, Altekruse SF, et al. Future of testicular germ cell tumor incidence in the United States: Forecast through 2026. Cancer. 2017;123(12):2320–2328. doi:10.1002/cncr.30597.
19.
Escobar D, Daneshmand S. Disparities in Testicular Cancer: A Review of the Literature. Cancers (Basel). 2024;16(20):3433. doi:10.3390/cancers16203433.
20.
Küronya Z, Fröhlich G, Ladányi A, et al. Low socioeconomic position is a risk factor for delay to treatment and mortality of testicular cancer patients in Hungary, a prospective study. BMC Public Health. 2021;21(1):1707. doi:10.1186/s12889-021-11720-w.
21.
Franco APS, Lima Figueiredo ER, Melo GS, et al. Predictors of Testicular Cancer Mortality in Brazil: A 20-Year Ecological Study. Cancers (Basel). 2023;15(16):4149. doi:10.3390/cancers15164149.
22.
Benjamin DJ, Shrestha A, Fellman D, Kalebasty AR. Trends in incidence and demographics of testicular cancer in California, 2000–2020. BJUI Compass. 2024;5(12):1249–1251. doi:10.1002/bco2.451.
23.
Fung C, Dinh PC, Fossa SD, Travis LB. Testicular Cancer Survivorship. J Natl Compr Canc Netw. 2019;17(12):1557–1568. doi:10.6004/jnccn.2019.7369.
24.
Smith ZL, Werntz RP, Eggener SE. Testicular Cancer: Epidemiology, Diagnosis, and Management. Med Clin North Am. 2018;102(2):251–264. doi:10.1016/j.mcna.2017.10.003.
25.
Fosså SD, Åbyholm T, Aakvaag A. Spermatogenesis and Hormonal Status after Orchiectomy for Cancer and before Supplementary Treatment. Eur Urol. 1984;10:173–177.
26.
Polish National Cancer Registry database. URL: https://onkologia.org.pl/pl/ra... (accessed: 2025.11.20).
27.
Kaczmarek T, Marcinkowski J, Szozda R, et al. The quality of the medical records seen from the perspective of needs of the Institution of Social Securities. Orzecznictwo Lek. 2010;7(1):66–73.
28.
Polish Supreme Audit Office (Najwyższa Izba Kontroli). Raport: System Ochrony Zdrowia w Polsce – stan obecny i pożądane kierunki zmian. (KZD.034.001.2018). Warszawa, 2019. URL: https://www.nik.gov.pl/plik/id... (accessed: 2025.11.20).
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.