RESEARCH PAPER
Patients’ preferences – evaluation of teleconsultations during the COVID-19 pandemic
1
Student Scientific Circle of Medical Communication, Medical University, Gdańsk, Poland
2
Department of Sociology of Medicine and Social Pathology, Medical University, Gdańsk, Poland
Corresponding author
Krzysztof Sobczak
Department of Sociology of Medicine and Social Pathology, Medical University, Gdańsk, Poland
Department of Sociology of Medicine and Social Pathology, Medical University, Gdańsk, Poland
Med Og Nauk Zdr. 2023;29(2):104-109
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
The COVID-19 pandemic caused necessary changes to the health care system in terms of the organization and treatment of patients. Remote forms of medical consultations were widely introduced to minimize the risk of viral transmission. The aim of the study was to assess patients’ opinions about teleconsultations during the COVID-19 pandemic regarding the doctor-patient relationship and communication.
Material and methods:
The study was conducted using a quantitative method with the CAWI technique, involving 1,011 adult patients consulted by their family physicians. Pearson’s chi-squared test was used to calculate statistical correlations for p < 0.05.
Results:
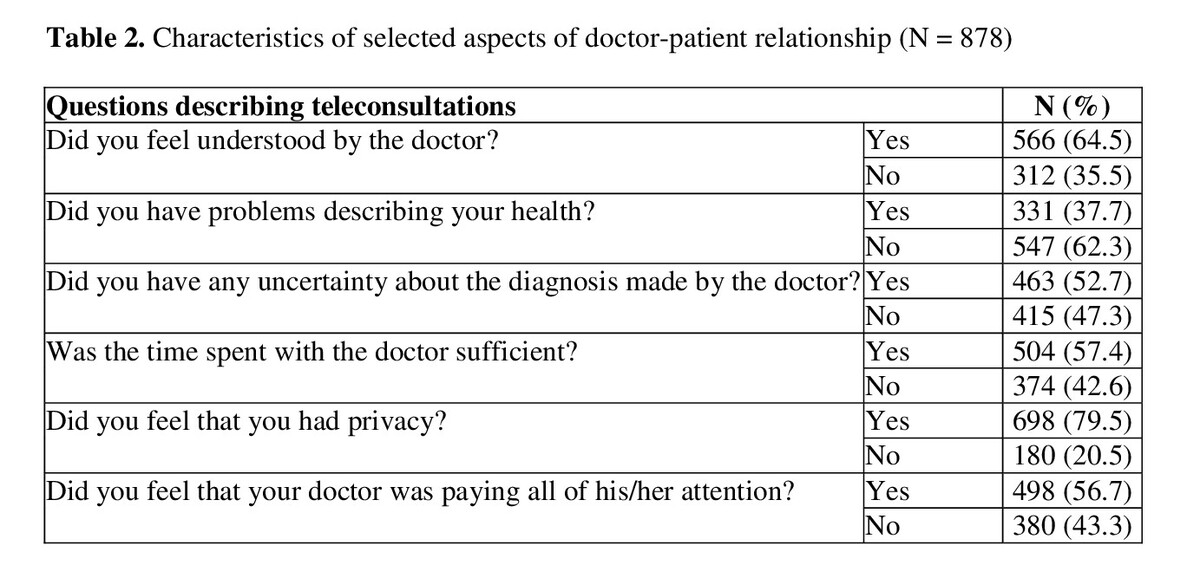
Overall, 46.4% of the respondents favourably evaluated the quality of communication during teleconsultations, while 28.2% of patients expressed negative opinions. A positive assessment of the quality of teleconsultation correlated with male gender, higher education, and living in large cities. As much as 43.3% of patients reported concerns about the doctor’s lack of attention experienced during remote consultations. As many as 33% (N = 290) of the respondents reported that remote consultations resulted in a re-evaluation of their trust in the doctor.
Conclusions:
Communication barriers during teleconsultations may lead to a limited understanding of the doctor’s message and recommendations. Their elimination and improved communication with patients can be an effective way to improve the level of service and facilitate access to family doctors’ services. The results can contribute to improving the functioning of health institutions, improving the quality of services, and increasing patient satisfaction.
The COVID-19 pandemic caused necessary changes to the health care system in terms of the organization and treatment of patients. Remote forms of medical consultations were widely introduced to minimize the risk of viral transmission. The aim of the study was to assess patients’ opinions about teleconsultations during the COVID-19 pandemic regarding the doctor-patient relationship and communication.
Material and methods:
The study was conducted using a quantitative method with the CAWI technique, involving 1,011 adult patients consulted by their family physicians. Pearson’s chi-squared test was used to calculate statistical correlations for p < 0.05.
Results:
Overall, 46.4% of the respondents favourably evaluated the quality of communication during teleconsultations, while 28.2% of patients expressed negative opinions. A positive assessment of the quality of teleconsultation correlated with male gender, higher education, and living in large cities. As much as 43.3% of patients reported concerns about the doctor’s lack of attention experienced during remote consultations. As many as 33% (N = 290) of the respondents reported that remote consultations resulted in a re-evaluation of their trust in the doctor.
Conclusions:
Communication barriers during teleconsultations may lead to a limited understanding of the doctor’s message and recommendations. Their elimination and improved communication with patients can be an effective way to improve the level of service and facilitate access to family doctors’ services. The results can contribute to improving the functioning of health institutions, improving the quality of services, and increasing patient satisfaction.
REFERENCES (37)
1.
Guo YR, Cao QD, Hong ZS, Tan YY, Chen SD, Jin HJ, et al. The origin, transmission and clinical therapies on coronavirus disease 2019 (COVID-19) outbreak – an update on the status. Mil Med Res. 2020;7(1):11.
2.
Pinkas J, Jankowski M, Szumowski Ł, Lusawa A, Zgliczyński WS, Raciborski F, et al. Public Health Interventions to Mitigate Early Spread of SARS-CoV-2 in Poland. Med Sci Monit. 2020;26:e924730.
3.
Pan XB. Application of personal-oriented digital technology in preventing transmission of COVID-19, China. Ir J Med Sci. 2020;189(4):1145–6.
4.
Amparore D, Campi R, Checcucci E, Sessa F, Pecoraro A, Minervini A, et al. Forecasting the Future of Urology Practice: A Comprehensive Review of the Recommendations by International and European Associations on Priority Procedures During the COVID-19 Pandemic. Eur Urol Focus. 2020;6(5):1032–48.
5.
Bujnowska-Fedak MM, Puchała E, Steciwko A. The impact of telehome care on health status and quality of life among patients with diabetes in a primary care setting in Poland. Telemed J E Health. 2011;17(3):153–63.
6.
Piotrowicz R, Krzesinski P, Balsam P, Piotrowicz E, Kempa M, Lewicka E, et al. Telemedicine solutions in cardiology. Kardiologia Polska. 2021;79(2).
7.
Ustawa z dnia 2 marca 2020 r. o szczególnych rozwiązaniach związanych z zapobieganiem, przeciwdziałaniem i zwalczaniem COVID-19, innych chorób zakaźnych oraz wywołanych nimi sytuacji kryzysowych (Dz.U. z 2021 r. poz. 2095).
8.
Ustawa z dnia 31 marca 2020 r. o zmianie niektórych ustaw w zakresie systemu ochrony zdrowia związanych z zapobieganiem, przeciwdziałaniem i zwalczaniem COVID-19 (Dz.U. 2020 poz. 567).
9.
Wrześniewska-Wal I, Hajdukiewicz D. Telemedycyna w Polsce – aspekty prawne, medyczne i etyczne. Studia Prawnoustrojowe. 2020;(50):509-24. https://doi.org/10.31648/sp.60...
10.
Healthcare. Telekonsultacje już powszechne: czy odpowiadają potrzebom pacjentów? Healthcare 2021. https://healthcaremarketexpert... (access: 27.01.2023)
11.
Biostat. Bezpieczeństwo zdrowotne w czasie pandemii koronawirusa. Biostat 2020. https://www.biostat.com.pl/bez... (access: 27.01.2023)
12.
Waller M, Stotler C. Telemedicine: a Primer. Curr Allergy Asthma Rep. 2018;18(10):54.
13.
Latifi R, Doarn CR. Perspective on COVID-19: Finally, Telemedicine at Center Stage. Telemed JE Health. 2020;26(9):1106–9.
14.
Weinstein RS, Lopez AM, Joseph BA, Erps KA, Holcomb M, Barker GP, et al. Telemedicine, telehealth, and mobile health applications that work: opportunities and barriers. Am J Med. 2014;127(3):183–7.
15.
Layfield E, Triantafillou V, Prasad A, Deng J, Shanti RM, Newman JG, et al. Telemedicine for head and neck ambulatory visits during COVID-19: Evaluating usability and patient satisfaction. Head Neck. 2020;42(7):1681–9.
16.
Florin M, Pinar U, Chavigny E, Bouaboula M, Jarboui L, Coulibaly A, et al. Socio-economic and psychological impact of the COVID-19 outbreak on private practice and public hospital radiologists. Eur J Radiol. 2020;132:109285.
17.
Ramaswamy A, Yu M, Drangsholt S, Ng E, Culligan PJ, Schlegel PN, et al. Patient Satisfaction With Telemedicine During the COVID-19 Pandemic: Retrospective Cohort Study. J Med Internet Res. 2020;22(9):e20786.
18.
Snoswell CL, Taylor ML, Comans TA, Smith AC, Gray LC, Caffery LJ. Determining if Telehealth Can Reduce Health System Costs: Scoping Review. J Med Internet Res. 2020;22(10):e17298.
19.
Le T, Toscani M, Colaizzi J. Telepharmacy: A New Paradigm for Our Profession. J Pharm Pract. 2020;33(2):176–82.
20.
Burke BL, Hall RW, CARE SOT. Telemedicine: Pediatric Applications. Pediatrics. 2015;136(1):e293–308.
21.
Ting L, Wilkes M. Telemedicine for Patient Management on Expeditions in Remote and Austere Environments: A Systematic Review. Wilderness Environ Med. 2021;32(1):102–11.
22.
Colbert GB, Venegas-Vera AV, Lerma EV. Utility of telemedicine in the COVID-19 era. Rev Cardiovasc Med. 2020;21(4):583–7.
23.
Hincapié MA, Gallego JC, Gempeler A, Piñeros JA, Nasner D, Escobar MF. Implementation and Usefulness of Telemedicine During the COVID-19 Pandemic: A Scoping Review. J Prim Care Community Health. 2020;11:2150132720980612.
24.
White SJ, Nguyen A, Roger P, Tse T, Cartmill JA, Willcock SM. Experiences of telehealth in general practice in Australia: research protocol for a mixed-methods study. BJGP Open. 2022;6(1):BJGPO.2021.0187.
25.
Zhou Y, Ma Y, Yang WFZ, Wu Q, Wang Q, Wang D, et al. Doctor-patient relationship improved during COVID-19 pandemic, but weakness remains. BMC Fam Pract. 2021;22(1):255.
26.
Berg M. Patient education and the physician-patient relationship. J Fam Pract. 1987;24(2):169–72.
27.
Imlach F, McKinlay E, Middleton L, Kennedy J, Pledger M, Russell L, et al. Telehealth consultations in general practice during a pandemic lockdown: survey and interviews on patient experiences and preferences. BMC Fam Pract. 2020;21(1):269.
28.
Carrillo de Albornoz S, Sia KL, Harris A. The effectiveness of teleconsultations in primary care: systematic review. Fam Pract. 2022;39(1):168–82.
29.
Haleem A, Javaid M, Singh RP, Suman R. Telemedicine for healthcare: Capabilities, features, barriers, and applications. Sens Int. 2021;2:100117.
30.
Mubaraki AA, Alrabie AD, Sibyani AK, Aljuaid RS, Bajaber AS, Mubaraki MA. Advantages and disadvantages of telemedicine during the COVID-19 pandemic era among physicians in Taif, Saudi Arabia. Saudi Med J. 2021;42(1):110–5.
31.
Gruppen LD, Wolf FM, Billi JE. Information gathering and integration as sources of error in diagnostic decision making. Med Decis Making. 1991;11(4):233–9.
32.
Vilendrer S, Sackeyfio S, Akinbami E, Ghosh R, Luu JH, Pathak D, et al. Patient Perspectives of Inpatient Telemedicine During the COVID-19 Pandemic: Qualitative Assessment. JMIR Form Res. 2022;6(3):e32933.
33.
Benis A, Banker M, Pinkasovich D, Kirin M, Yoshai BE, Benchoam-Ravid R, et al. Reasons for Utilizing Telemedicine during and after the COVID-19 Pandemic: An Internet-Based International Study. J Clin Med. 2021;10(23).
34.
Clark PA, Capuzzi K, Harrison J. Telemedicine: medical, legal and ethical perspectives. Med Sci Monit. 2010;16(12):RA261–72.
35.
Chipidza FE, Wallwork RS, Stern TA. Impact of the Doctor-Patient Relationship. Prim Care Companion CNS Disord. 2015;17(5).
36.
Proulx-Cabana S, Segal TY, Gregorowski A, Hargreaves D, Flannery H. Virtual Consultations: Young People and Their Parents' Experience. Adolesc Health Med Ther. 2021;12:37–43.
37.
Scott Kruse C, Karem P, Shifflett K, Vegi L, Ravi K, Brooks M. Evaluating barriers to adopting telemedicine worldwide: A systematic review. J Telemed Telecare. 2018;24(1):4–12.
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.