RESEARCH PAPER
Assessment of illness acceptance and satisfaction with life in patients with inflammatory bowel diseases, taking into account sociodemographic and clinical factors
1
Katedra Nauk Społecznych i Medycznych, Wydział Nauk o Zdrowiu, Uniwersytet Mikołaja Kopernika w Toruniu Collegium Medicum w Bydgoszczy, Polska
2
10 Wojskowy Szpital Kliniczny z Polikliniką w Bydgoszczy, Polska
Corresponding author
Halina Zielińska-Więczkowska
Katedra Nauk Społecznych i Medycznych, Wydział Nauk o Zdrowiu, Uniwersytet Mikołaja Kopernika w Toruniu Collegium Medicum w Bydgoszczy, ul. Świętojańska 20, 85-077, Bydgoszcz, Polska
Katedra Nauk Społecznych i Medycznych, Wydział Nauk o Zdrowiu, Uniwersytet Mikołaja Kopernika w Toruniu Collegium Medicum w Bydgoszczy, ul. Świętojańska 20, 85-077, Bydgoszcz, Polska
Med Og Nauk Zdr. 2021;27(3):306-311
KEYWORDS
TOPICS
ABSTRACT
Introduction and objective:
Non-specific inflammatory bowel diseases are chronic, lifelong conditions which require medical attention. This health problem often concerns young people. The aim of the study was to assess the level of illness acceptance and satisfaction with life in patients with non-specific inflammatory bowel diseases, including Leśniowski-Crohn’s disease (CD) and ulcerative colitis (UC), and indication of relationships with sociodemographic and clinical factors.
Material and methods:
The study included 90 patients of Clinical Gastroenterology Ward and Bowel Disease Clinic located in two hospitals in Bydgoszcz. All patients were over the age of 18 years. A diagnostic survey was used along with the Acceptance of Illness Scale (AIS) and Satisfaction With Life Scale (SWLS), and an author constructed questionnaire containing sociodemographic and clinical data.
Results:
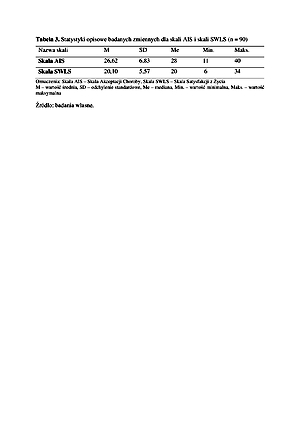
Mean score was 26.62±6.83 for AIS and 20.10±5.57 for SWLS. A correlation was observed between the level of illness acceptance and satisfaction with life (r = 0.60; p < 0.001). Males showed a significantly higher level of illness acceptance than females (28.20±6.33 vs. 25.11±7.01; p = 0.031). The occurrence of the symptoms of disease and the phase of disease exacerbation decreased the level of illness acceptance and the sense of satisfaction with life. No significant differences between the AIS and SWLS scores were observed according to the type of disease.
Conclusions:
The participants of the study showed an average level of illness acceptance and satisfaction with life. Patients who accepted their disease were more satisfied with life. Asymptomatic patients whose condition was in remission had higher scores on AIS and SWLS.
Non-specific inflammatory bowel diseases are chronic, lifelong conditions which require medical attention. This health problem often concerns young people. The aim of the study was to assess the level of illness acceptance and satisfaction with life in patients with non-specific inflammatory bowel diseases, including Leśniowski-Crohn’s disease (CD) and ulcerative colitis (UC), and indication of relationships with sociodemographic and clinical factors.
Material and methods:
The study included 90 patients of Clinical Gastroenterology Ward and Bowel Disease Clinic located in two hospitals in Bydgoszcz. All patients were over the age of 18 years. A diagnostic survey was used along with the Acceptance of Illness Scale (AIS) and Satisfaction With Life Scale (SWLS), and an author constructed questionnaire containing sociodemographic and clinical data.
Results:
Mean score was 26.62±6.83 for AIS and 20.10±5.57 for SWLS. A correlation was observed between the level of illness acceptance and satisfaction with life (r = 0.60; p < 0.001). Males showed a significantly higher level of illness acceptance than females (28.20±6.33 vs. 25.11±7.01; p = 0.031). The occurrence of the symptoms of disease and the phase of disease exacerbation decreased the level of illness acceptance and the sense of satisfaction with life. No significant differences between the AIS and SWLS scores were observed according to the type of disease.
Conclusions:
The participants of the study showed an average level of illness acceptance and satisfaction with life. Patients who accepted their disease were more satisfied with life. Asymptomatic patients whose condition was in remission had higher scores on AIS and SWLS.
REFERENCES (23)
1.
Alarhayem A, Achebe E, Logue A. Psychosocial support of the in-flammatory bowel disease patient. Surg Clin North Am. 2015; 95(6): 1281–1293. http://dx.doi.org/10.1016/j.su....
2.
Ilias T, Bungau S, Tit DM, et al. Psychosocial profile of the patients with inflammatory bowel disease. Exp Ther Med. 2020; 20(3): 2493–2500. https://doi.org/10.3892/etm.20....
3.
Prabha GS, Srinivasan N, Aravindh S, et al. Study on quality of life in patients with inflammatory bowel diseases (IBD): impact of sociodemo-graphic factors. Int J Pharm Sci Res. 2020; 34: 2823–2827. doi: 10.13040/IJPSR.0975-8232.11(6).2823-27.
4.
Sarwan N, Jurawan R, Singh R, et al. An exploratory study of inflamma-tory bowel disease and the psychosocial factors affecting health-related quality of life. Med Sci. (Basel). 2019; 7(2), 18. https://doi.org/10.3390/medsci....
5.
Miklas N, Szostkowska M, Zdrojewski Z. Seksualność kobiet z nie-swoistymi chorobami zapalnymi jelit – badania własne. Seksuologia Polska 2015; 13(2): 45–52.
6.
Hagelund LM, Stallknecht SE, Jensen HM. Quality of life and patients preferences among Danish patients with ulcerative colitis – results from a survey study. Curr Med Res Opin. 2020; 36(5): 771–779. https://doi.org/1080/03007995.....
7.
Cepuch G, Śniadek A, Śręba S. Jakość życia młodzieży z chorobą Leś-niowskiego-Crohna. Med. Og Nauk Zdr. 2015; 21(4): 352–356. doi: 10.5604/20834543.1186904.
8.
Chrobak-Bień J, Gawor A, Paplaczyk M, Gąsiorowska A. Wpływ czynni-ków socjodemograficznych i klinicznych na stopień akceptacji choroby wśród osób cierpiących na chorobę Leśniowskiego-Crohna. Piel Zdr Publ. 2018; 8(1): 47–53.
9.
Chrobak-Bień J, Gawor A, Paplaczyk M, Gąsiorowska A. Analysis of fac-tors affecting the quality of life of those suffering from Crohn's disease. Pol Przegl Chir. 2017; 89(4): 16–22. doi: 10.5604/01.300010010.3904.
10.
Glinkowski S, Marcinkowska D. Wrzodziejące zapalenie jelita grubego – ocena aktywności choroby na podstawie współcześnie stosowanych skal. Nowa Med. 2018; 3: 123–137. doi: 10.25121/NM.2018.25.3.123.
11.
Chrobak-Bień J, Gawor A, Paplaczyk M, Małecka-Panas E, Gąsiorow-ska A. Wpływ akceptacji choroby na jakość życia pacjentów z chorobą Leśniowskiego-Crohna. Nowa Med. 2017; 24(1): 5–17.
12.
Magalhães J, de Castro FD, Carvalho PB, Moreira MJ, Cotter J. Quality of life patients with inflammatory bowel disease: importance of clinical, demographic and psychosocial factors. Arq Gastroenterol. 2014; 51(3). https://dx.doi.org/10.1590/S00....
13.
Pittet V, Vaucher C, Froehlich F, et al. Patient self-reported concerns in inflammatory bowel diseases: A gender-specific subjective quality-of-life indicator. PLoS ONE. 2017; 12(2): E0171864. https://doi.org/10.1371/journa....
14.
Taft TH, Ballou S, Bedell A, et al. Psychological considerations and interventions in inflammatory bowel disease patient care. Gastroenterol Clin North Am. 2017; 46(4): 847–858. doi: 10.1016/j.gtc.2017.08.007.
15.
Glińska J, Grzegorczyk A, Dziki Ł, Dziki A. Proces adaptacji do życia z nieswoistymi chorobami zapalnymi jelit. Probl Pielęg. 2015; 23(1): 7–12. doi: 10.5603/PP.2015.0002.
16.
Casellas F, Ginard D, Vera I, Torrejon A. Satisfaction of health care professionals managing patients with inflammatory bowel disease. J Crohns Colitis 2013; 7(7): e249–e255.
17.
Berding A, Witte C, Gottschald M, Kaltz B, Weiland R, Gerlich C, Re-usch A, Kruis W, Faller H. Beneficial effects of education on emotional distress, self-management, and coping in patients with inflammatory bowel disease: a prospective randomized controlled study. Inflamm Intest Dis. 2016; 1: 182–190. https://doi.org/10.1159/000452....
18.
Juczyński Z. Narzędzia pomiaru w promocji i psychologii zdrowia. Warszawa: Pracownia Testów Psychologicznych Polskiego Towarzystwa Psychologicznego; 2012.
19.
Cioffi I, Imperatore N, Di Vincenzo O, et al. Association between health-related quality of life and nutritional status in adult patients with Crohn's disease. Nutrients. 2020; 12(3): 746. https://doi.org/10.3390/nu1203....
20.
Habidi F, Habidi ME, Gharavimia A, et al. Quality of life in inflam-matory bowel disease patients: A cross-sectional study. J Res Med Sci. 2017; 22:104. doi: 10.4103/jrms.JRMS_975_16.
21.
Have M, Aalst, Kaptein AA, et al. Determinants of health-related quality of life in Crohn's disease: A systematic review and meta-ana-lysis. J Crohns Colitis. 2014; 8: 93–106. http://dx.doi.org/10.1016/j.cr....
22.
Stapersma L, van den Brink G, van der Ende J, Bodelier AG, van Wering HM, Hurkmans PC, Mearin ML, van der Meulen-de Jong AE, Escher JC, Utens E. Illness perception and depression are associated with health-related quality of life in youth with inflammatory bowel disease. Int J Behav Med. 2019; 26: 415–426. doi: 10.1007/s12529-019-09791-6.
23.
Kozłowska K, Bączyk G, Krokowicz P. Quality of life in patients with ul-cerative colitis treated surgically. Prz Gastroenterol. 2014; 9(4): 220–226. doi: 10.5114/pg.2014.45104.
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.