RESEARCH PAPER
Lifestyle and psychosocial risks among women with polycystic ovary syndrome and insulin resistance
1
Studenckie Koło Naukowe Dietetyki przy Zakładzie Żywienia Klinicznego i Diagnostyki Gastroenterologicznej, Uniwersytet Medyczny w Łodzi, Polska
2
Zakład Żywienia i Epidemiologii, Uniwersytet Medyczny w Łodzi, Polska
3
Zakład Epidemiologii i Biostatystyki, Uniwersytet Medyczny w Łodzi, Polska
Corresponding author
Katarzyna Stańczyk
Studenckie Koło Naukowe Dietetyki przy Zakładzie Żywienia Klinicznego i Diagnostyki Gastroenterologicznej, Uniwersytet Medyczny w Łodzi, Łódź, Polska
Studenckie Koło Naukowe Dietetyki przy Zakładzie Żywienia Klinicznego i Diagnostyki Gastroenterologicznej, Uniwersytet Medyczny w Łodzi, Łódź, Polska
Med Og Nauk Zdr. 2021;27(3):312-317
KEYWORDS
insulin resistancelifestylehealth behaviourshirsutismpsychosocial factorspolycystic ovary syndrome (PCOS)
TOPICS
ABSTRACT
Introduction and objective:
PCOS is the most commonly diagnosed endocrine disorder among women at reproductive age, often accompanied by insulin resistance (IR). Symptoms of PCOS result in a reduction of the quality of life and psychosocial well-being of the patients. The aim of the study was to assess the selected elements of lifestyle and the presence of psychosocial risks among adult women with PCOS and IR.
Material and methods:
The study included 60 women aged 18–35. The author constructed questionnaire was made available electronically among women under care of the Insulin Resistance Foundation – a healthy diet and a healthy life. The modified Ferriman-Gallwey scale was used to quantify the severity of hirsutism. Nutritional status was diagnosed based on WHO standards (BMI). Statistical analysis was performed using chi 2 test for independence, Mann-Whitney U test and Shapiro-Wilk test. Structural indicators were analyzed in fractions.
Results:
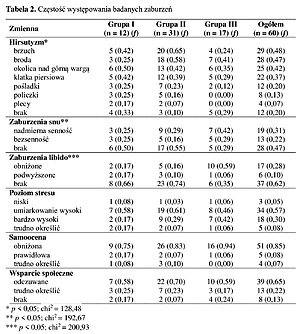
Excess body weight was observed in over a half of the patients (f=0.55). More than half of the respondents experienced sleep disorders, and 1/3 libido disorders. In 8 out of 10 patients hirsutism was reported. The majority of respondents experienced a decline in self-esteem (f = 0.85), simultaneously more than 1/3 of them did not feel any social support. Almost 9 out of 10 women reported high or moderate levels of perceived stress. Over 1/3 of the surveyed women (f = 0.38) consumed alcohol at least several times a month.
Conclusions:
The presence of health disorders diagnosed as a part of PCOS, including hirsutism, may exacerbate the risks that hinder the psychosocial functioning of the women. In combination with negative lifestyle patterns, this leads to a reduction in the quality of life.
PCOS is the most commonly diagnosed endocrine disorder among women at reproductive age, often accompanied by insulin resistance (IR). Symptoms of PCOS result in a reduction of the quality of life and psychosocial well-being of the patients. The aim of the study was to assess the selected elements of lifestyle and the presence of psychosocial risks among adult women with PCOS and IR.
Material and methods:
The study included 60 women aged 18–35. The author constructed questionnaire was made available electronically among women under care of the Insulin Resistance Foundation – a healthy diet and a healthy life. The modified Ferriman-Gallwey scale was used to quantify the severity of hirsutism. Nutritional status was diagnosed based on WHO standards (BMI). Statistical analysis was performed using chi 2 test for independence, Mann-Whitney U test and Shapiro-Wilk test. Structural indicators were analyzed in fractions.
Results:
Excess body weight was observed in over a half of the patients (f=0.55). More than half of the respondents experienced sleep disorders, and 1/3 libido disorders. In 8 out of 10 patients hirsutism was reported. The majority of respondents experienced a decline in self-esteem (f = 0.85), simultaneously more than 1/3 of them did not feel any social support. Almost 9 out of 10 women reported high or moderate levels of perceived stress. Over 1/3 of the surveyed women (f = 0.38) consumed alcohol at least several times a month.
Conclusions:
The presence of health disorders diagnosed as a part of PCOS, including hirsutism, may exacerbate the risks that hinder the psychosocial functioning of the women. In combination with negative lifestyle patterns, this leads to a reduction in the quality of life.
REFERENCES (48)
1.
Azziz R, Woods KS, Reyna R, et al. The prevalence and features of the polycystic ovary syndrome in an unselected population. J Clin Endocrinol Metab. 2004; 89(6): 2745–2749. https://doi.org/10.1210/jc.200....
2.
Rodrigues-Paris D, Remlinger-Molenda A, Kurzawa R, et al. Występowanie zaburzeń psychicznych u kobiet z zespołem policystycznych jajników. Psychiatr Pol. 2019; 130: 1–12. https://doi.org/10.12740/PP/On....
3.
Sengupta S, Jaseem T, Ambalavanan J, et al. Homeostatic Model Assessment-Insulin Resistance (HOMA-IR 2) in Mild Subclinical Hypothyroid Subjects. Indian J Clin Biochem. 2018; 33(2): 214–217. https://doi.org/10.1007/s12291....
4.
Meigs JB. Epidemiology of the insulin resistance syndrome. Curr Diab Rep. 2003; 3(1): 73–9. https://doi.org/10.1007/s11892....
5.
Płaczkowska S, Pawlik-Sobecka L, Kokot I, et al. Analiza częstości występowania insulinooporności u osób młodych w oparciu o wybrane kryteria diagnostyczne – badanie wstępne. Hygeia Public Health 2014; 49(4): 851–856. https://www.h-ph.pl/hyg.php?op... (access: 2021.04.28).
6.
Bermudez V, Salazar J, Martínez MS, et al. Prevalence and Associated Factors of Insulin Resistance in Adults from Maracaibo City, Venezuela. Adv Prev Med. 2016; 2016: 9405105. https://doi.org/10.1155/2016/9....
7.
Al-Jefout M, Alnawaiseh N, Al-Qtaitat A. Insulin resistance and obesity among infertile women with different polycystic ovary syndrome pheno -types. Sci Rep. 2017; 7: 5339. https://doi.org/10.1038/s41598....
8.
Gutch M, Kumar S, Razi SM, et al. Assessment of insulin sensitivity/resistance. Indian J Endocrinol Metab. 2015; 19(1): 160–164. https://doi.org/ 10.4103/2230-8210.146874.
9.
Rotterdam ESHRE/ASRM-Sponsored PCOS Consensus Workshop Group, Revised 2003 consensus on diagnostic criteria and long-term health risks related to polycystic ovary syndrome (PCOS). Hum Reprod. 2004; 19(1): 41–47. https://doi.org/10.1093/humrep....
10.
Greenwood EA, Pasch LA, Cedars MI, et al. Insulin Resistance is Associated with Depression Risk in Polycystic Ovary Syndrome. Fertil Steril. 2018; 110(1): 27–34. https://doi.org/10.1016/j.fert....
11.
Alur-Gupta S, Chemerinski A, Liu C, et al. Body image distress increased in women with PCOS and mediates depression and anxiety. Fertil Steril. 2019; 112(5): 930–938.e1. https://doi.org/10.1016/j.fert....
12.
Ferriman D, Purdie AW. Association of oligomenorrhoea, hirsuties, and infertility. Br Med J. 1965; 2(5453): 69–72. https://doi.org/10.1136/bmj.2.....
13.
World Health Organization. Nutrition Landscape Information System (NLIS) country profile indicators: interpretation guide. 2010; 3. ISBN: 9789241599955.
14.
Khomami MB, Tehrani FR, Hashemi S, et al. Of PCOS Symptoms, Hirsutism Has the Most Significant Impact on the Quality of Life of Iranian Women. PLoS One. 2015; 10(4): e0123608. https://doi.org/10.1371/journa....
15.
Rzońca E, Bień A, Wdowiak A, et al. Determinants of Quality of Life and Satisfaction with Life in Women with Polycystic Ovary Syndrome. Int J Environ Res Public Health. 2018; 15(2): 376. https://doi.org/10.3390/ijerph....
16.
Sánchez-Ferrer ML, Adoamnei E, Prieto-Sánchez MT, et al. Health-related quality of life in women with polycystic ovary syndrome attending to a tertiary hospital in Southeastern Spain: a case-control study. Health and Quality of Life Outcomes 2020; 18(1): 232. https://doi.org/10.1186/s12955....
17.
Chaudhari AP, Mazumdar K, Mehta PD. Anxiety, Depression, and Quality of Life in Women with Polycystic Ovarian Syndrome. Indian J Psychol Med. 2018; 40(3): 239–246. https://doi.org/10.4103/IJPSYM....
18.
Fliegner M, Richter-Appelt H, Krupp K, et al. Sexual Function and Socio-Sexual Difficulties in Women with Polycystic Ovary Syndrome (PCOS). Geburtshilfe Frauenheilkd. 2019; 79(5): 498–509. https://doi.org/10.1055/a-0828....
19.
Zhang B, Zhou W, Shi Y, et al. Lifestyle and environmental contributions to ovulatory dysfunction in women of polycystic ovary syndrome.\ BMC Endocr Disord. 2020; 20(1): 19. https://doi.org/10.1186/s12902....
20.
Bazarganipour F, Ziaei S, Montazeri A, et al. Body image satisfaction and self-esteem status among the patients with polycystic ovary syndrome. Iran J Reprod Med. 2013; 11(10): 829–836. http://journals.ssu.ac.ir/ijrm... (access: 2021.03.30).
21.
Sidra S, Tariq MH, Farrukh MJ, et al. Evaluation of clinical manifestations, health risks, and quality of life among women with polycystic ovary syndrome. PLoS One. 2019; 14(10): e0223329. https://doi.org/10.1371/journa....
22.
Hadjiconstantinou M, Mani H, Patel N, et al. Understanding and supporting women with polycystic ovary syndrome: a qualitative study in an ethnically diverse UK sample. Endocr Connect. 2017; 6(5): 323–330. https://doi.org/10.1530/EC-17-....
23.
Hahn S, Janssen OE, Tan S, et al. Clinical and psychological correlates of quality-of-life in polycystic ovary syndrome. Eur J Endocrinol. 2005; 153: 853–60. https://doi.org/10.1530/eje.1.....
24.
Taghavi SA, Bazarganipour F, Hugh-Jones S, et al. Health-related quality of life in Iranian women with polycystic ovary syndrome: a qualitative study. BMC Womens Health. 2015; 15: 111. https://doi.org/10.1186/s12905....
25.
Amiri FN, Tehrani FR, Simbar M, et al. Female Gender Scheme is Disturbed by Polycystic Ovary Syndrome: A Qualitative Study From Iran. Iran Red Crescent Med J. 2014; 16(2): e12423. https://doi.org/10.5812/ircmj.....
26.
Kitzinger C, Willmott J. ‹The thief of womanhood›: women›s experience of polycystic ovarian syndrome. Soc Sci Med. 2002; 54(3): 349–61. https://doi.org/10.1016/s0277-....
27.
Dashti S, Latiff LA, Hamid HA, et al. Sexual Dysfunction in Patients with Polycystic Ovary Syndrome in Malaysia. Asian Pac J Cancer Prev. 2016; 17(8): 3747–51. http://journal.waocp.org/artic... (dostęp: 2021.03.30).
28.
Moran LJ, March WA, Whitrow MJ, et al. Sleep disturbances in a community-based sample of women with polycystic ovary syndrome. Human Reprod. 2015; 30(2): 466–472. https://doi.org/10.1093/humrep....
29.
Naqvi SH, Moore A, Bevilacqua K, et al. Predictors of depression in women with polycystic ovary syndrome. Arch Womens Ment Health. 2015; 18(1): 95–101. https://doi.org/10.1007/s00737....
30.
Glidewell RN, McPherson Botts E, Orr WC. Insomnia and anxiety: diagnostic and management implications of complex interactions. Sleep Med Clin. 2015; 10(1): 93–99. https://doi.org/10.1016/j.jsmc....
31.
Sulaiman MAH, Al-Farsi YM, Al-Khaduri MM, et al. Psychological burden among women with polycystic ovarian syndrome in Oman: a case–control study. Int J Womens Health. 2017; 9: 897–904. https://doi.org/10.2147/IJWH.S....
32.
Kolahi L, Asemi N, Mirzaei M, et al. The relationship between quality of life and coping strategies in polycystic ovary syndrome patients. Adv Biomed Res. 2015; 4: 168. https://doi.org/10.4103/2277-9....
33.
Copp T, Hersch J, Muscat DM, et al. The benefits and harms of receiving a polycystic ovary syndrome diagnosis: a qualitative study of women’s experiences. Hum Reprod Open. 2019; 2019(4): hoz026. https://doi.org/10.1093/hropen....
34.
Martin ML, Halling K, Eek D, et al. Understanding polycystic ovary syndrome from the patient perspective: a concept elicitation patient interview study. Health Qual Life Outcomes. 2017; 15: 162. https://doi.org/10.1186/s12955....
35.
Ekbäck MP, Lindberg M, Benzein E, et al. Social support: an important factor for quality of life in women with hirsutism. Health Qual Life Outcomes. 2014; 12: 183. https://doi.org/10.1186/s12955....
36.
Wright PJ, Dawson RM, Corbett CF. Social construction of biopsychosocial and medical experiences of women with polycystic ovary syndrome. J Adv Nurs. 2020; 76(7): 1728–1736. https://doi.org/10.1111/jan.14....
37.
Holbrey S, Coulson NS. A qualitative investigation of the impact of peer to peer online support for women living with Polycystic Ovary Syndrome. BMC Womens Health. 2013; 13: 51. https://doi.org/10.1186/1472-6....
38.
Roessler KK, Glintborg D, Ravn P, et al. Supportive relationships-psychological effects of group counselling in women with polycystic ovary syndrome (PCOS). Commun Med. 2012; 9(2): 125–31. https://doi.org/10.1558/cam.v9....
39.
Jiskoot G, Dietz de Loos A, Beerthuizen A, et al. Long-term effects of a three-component lifestyle intervention on emotional well-being in women with Polycystic Ovary Syndrome (PCOS): A secondary analysis of a randomized controlled trial. PLoS One. 2020; 15(6): e0233876. https://doi.org/10.1371/journa....
40.
Basu BR, Chowdhury O, Saha SK. Possible Link Between Stress-related Factors and Altered Body Composition in Women with Polycystic Ovarian Syndrome. J Hum Reprod Sci. 2018; 11(1): 10–18. https://doi.org/10.4103/jhrs.J....
41.
Mohammadi M. Oxidative Stress and Polycystic Ovary Syndrome: A Brief Review. Int J Prev Med. 2019; 10: 86. https://doi.org/10.4103/ijpvm.....
42.
Damone AL, Joham AE, Loxton D, et al. Depression, anxiety and perceived stress in women with and without PCOS: a community-based study. Psychol Med. 2019; 49(9): 1510–1520. https://doi.org/10.1017/S00332....
43.
Zangeneh FZ, Jafarabadi M, Naghizadeh MM, et al. Psychological Distress in Women with Polycystic Ovary Syndrome from Imam Khomeini Hospital, Tehran. J Reprod Infertil. 2012; 13(2): 111–115. https://www.jri.ir/article/501 (access: 2021.03.30).
44.
Barry JA, Hardiman PJ, Saxby BK, et al. Testosterone and mood dysfunction in women with polycystic ovarian syndrome compared to subfertile controls. J Psychosom Obstet Gynaecol. 2011; 32(2): 104–11. https://doi.org/10.3109/016748....
45.
Peltier MR, Verplaetse TL, Mineur YS, et al. Sex differences in stress -related alcohol use. Neurobiol Stress. 2019; 10: 100149. https://doi.org/10.1016/j.ynst....
46.
Clay JM, Parker MO. The role of stress-reactivity, stress-recovery and risky decision-making in psychosocial stress-induced alcohol consumption in social drinkers. Psychopharmacology (Berl). 2018; 235(11): 3243–3257. https://doi.org/10.1007/s00213....
47.
Legro RS, Chen G, Kunselman AR, et al. Smoking in infertile women with polycystic ovary syndrome: baseline validation of self-report and effects on phenotype. Hum Reprod. 2014; 29(12): 2680–2686. https://doi.org/10.1093/humrep....
48.
Artese A, Stamford BA, Moffatt RJ. Cigarette Smoking: An Accessory to the Development of Insulin Resistance. Am J Lifestyle Med. 2019; 13(6): 602–605. https://doi.org/10.1177/155982....
Share
RELATED ARTICLE
We process personal data collected when visiting the website. The function of obtaining information about users and their behavior is carried out by voluntarily entered information in forms and saving cookies in end devices. Data, including cookies, are used to provide services, improve the user experience and to analyze the traffic in accordance with the Privacy policy. Data are also collected and processed by Google Analytics tool (more).
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.
You can change cookies settings in your browser. Restricted use of cookies in the browser configuration may affect some functionalities of the website.